Methods of Varicose Vein Treatment
Overview of Treatment Options Available at IVSI
Varicose vein treatment is not one-size-fits-all.
The most appropriate treatment for varicose veins depends on
symptoms, ultrasound findings, vein anatomy, and overall clinical assessment.
Not all patients require intervention.
Not all veins require the same type of treatment.
How Varicose Veins Are Treated
Modern treatment of varicose veins and chronic venous insufficiency (CVI) focuses on closing or removing abnormal superficial veins that no longer function properly.
These veins allow blood to flow backward (venous reflux), contributing to:
- Leg pain
- Swelling
- Heaviness
- Skin changes
- Visible bulging veins
Treatment methods are minimally invasive, performed in-office, and guided by ultrasound imaging.
The deep venous system — which carries the majority of blood flow from the legs — is preserved and never treated.
Conservative (Non‑Procedural) Management
Conservative care may be recommended:
- As an initial step
- When procedural treatment is not medically indicated
- When symptoms are mild
Common measures include:
- Graduated compression stockings
- Regular walking and leg movement
- Weight management and lifestyle modification
Conservative therapy may help relieve symptoms but does not eliminate diseased veins or correct venous reflux.
Minimally Invasive Varicose Vein Procedures
When medical criteria are met, minimally invasive procedures may be recommended to address malfunctioning superficial veins.
Treatment selection is determined by clinical findings and medical judgment, in accordance with accepted medical standards and applicable insurance medical necessity guidelines.
#1 Endovenous Laser Ablation (EVLA)
Also known as Endovenous Laser Treatment (EVLT), EVLA is a widely used treatment for varicose veins caused by axial vein reflux.
During this minimally invasive, in-office procedure:
- A thin laser fiber is inserted into the diseased vein through a small skin puncture
- Local anesthetic is administered along the vein to provide comfort and protect surrounding tissue
- Laser energy is delivered to close the vein
The treated vein is sealed, and blood flow is redirected into healthy veins.
EVLA is associated with durable vein closure and is commonly used for treatment of the great and small saphenous veins.
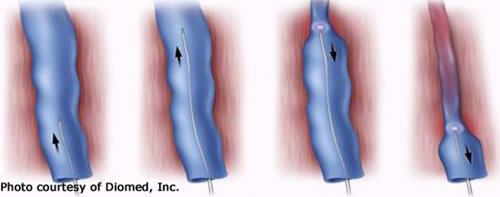
Illustration for educational purposes. Not an actual patient
👉 Learn more about Endovenous Laser Ablation (EVLA)
#2 Percutaneous Ablation of Perforating Veins (PAP)
Percutaneous Ablation of Perforating Veins (PAP) is used to treat incompetent perforator veins that allow abnormal blood flow between the superficial and deep venous systems.
During this ultrasound-guided procedure:
- A laser fiber is inserted through a small skin puncture
- Local anesthetic is administered around the targeted perforator vein
- Laser energy is delivered to close the incompetent perforator vein
- Abnormal cross-flow between the superficial and deep systems is eliminated
Laser ablation of perforating veins is technically demanding due to the small diameter and variable anatomical location of these veins.
Treatment is recommended only when perforator reflux is clearly contributing to symptoms or advanced skin changes.
#3 Ultrasound-Guided Sclerotherapy (Liquid)
Ultrasound-Guided Sclerotherapy uses real-time ultrasound imaging to guide injection of a liquid sclerosant into varicose veins that are not visible on the skin surface.
The sclerosant irritates the inner lining of the vein, causing it to collapse and gradually be reabsorbed by the body.
This technique may be appropriate for:
- Deeper varicosities not visible under the skin
- Residual veins following prior treatment
- Smaller tributary veins
Ultrasound guidance allows accurate placement of the sclerosant into targeted veins while avoiding surrounding structures.
👉 Learn more about Sclerotherapy for Varicose Veins
#4 Ultrasound-Guided Foam Sclerotherapy (UGFS)
Ultrasound-Guided Foam Sclerotherapy uses real-time ultrasound imaging to guide injection of a physician-prepared sclerosant foam into targeted veins.
The foam displaces blood within the vein and increases contact between the sclerosant and the vein wall, promoting vein closure and gradual resorption.
UGFS may be used for:
- Tortuous or irregular veins
- Tributary veins not suitable for thermal ablation
- Residual or recurrent varicose veins
- Selected axial veins in appropriate clinical situations
- Incompetent perforator veins when indicated
Foam sclerotherapy allows treatment of veins that are difficult to access with a laser fiber or catheter.
Treatment selection depends on vein size, anatomy, ultrasound findings, and overall clinical presentation.
#5 Varithena® (Polidocanol Injectable Microfoam)
Varithena® is an FDA-approved, commercially prepared microfoam formulation of polidocanol used to treat incompetent superficial veins.
Unlike physician-prepared foam, Varithena is manufactured to provide standardized foam characteristics and consistent concentration.
During the procedure:
- The microfoam is injected into the targeted vein under ultrasound guidance
- The foam displaces blood within the vein and irritates the vein lining
- The treated vein collapses and is gradually reabsorbed by the body
Varithena may be considered for:
- Incompetent great and accessory saphenous veins
- Recurrent varicose veins
- Patients in whom thermal ablation is not ideal
Treatment selection depends on vein anatomy, ultrasound findings, prior treatment history, and overall clinical assessment.
#6 Compression Sclerotherapy
The most common treatment for reticular veins and spider veins.
- Performed using very fine needles
- Sensation similar to a mosquito bite
- Multiple sessions may be required
Temporary bruising is common. Skin discoloration, if it occurs, typically fades over several months.
👉 Learn more about Sclerotherapy Injections for Spider Veins
#7 Ambulatory (Stab) Phlebectomy
A surgical technique used to remove large, bulging varicose veins through tiny skin openings.
- Small punctures usually do not require stitches
- Minimal scarring
- Immediate visual improvement
While once very popular, this procedure is now used selectively, as many veins can be treated effectively with foam sclerotherapy.
VNUS Closure (Radiofrequency Ablation)
Radiofrequency ablation was introduced in 1999 and predates laser technology. While still used by some physicians, it requires a larger, less flexible catheter.
Due to advancements in laser technology—particularly the 1470 nm diode laser—radiofrequency ablation is no longer offered at our clinic.
VenaSeal® (Medical Adhesive Closure)
VenaSeal® is an FDA-approved medical adhesive used to close veins. FDA approval does not mean a procedure is appropriate for every patient. Published medical literature has reported inflammatory and thromboembolic complications associated with cyanoacrylate vein closure.
Based on physician judgment, patient safety considerations, and long-term reliability, VenaSeal® is not offered at our clinic.
Reference:
Phlebology: The Journal of Venous Disease, October 30, 2023
Treatment Selection and Staging
The choice of treatment method depends on:
- Symptom severity
- Ultrasound findings
- Vein size and location
- Safety and clinical considerations
Varicose vein treatment is typically performed in stages:
- Treatment of primary refluxing veins
- Reassessment with ultrasound
- Additional targeted treatment if needed
Not all patients require procedural treatment, and not all veins require intervention.
In‑Office Care and Recovery
All procedures are:
- Performed in-office
- Done under local anesthesia only
- Do not require hospital admission
- Associated with rapid return to daily activity
Recovery recommendations vary depending on procedure and patient factors.
Schedule Your Varicose Vein Evaluation
If you are experiencing leg pain, swelling, heaviness, or visible veins, expert evaluation matters.
📞 Call (847) 518-9999 to schedule a vein evaluation
Medical Disclaimer
The information on this page is for educational purposes only and does
not substitute for professional medical advice, diagnosis, or treatment.
Treatment recommendations depend on a physician’s evaluation, diagnostic
testing, and individual patient circumstances.
Learn More